Editor’s note: J. Douglas Coatsworth, a professor in the Department of Human Development and Family Studies at Colorado State University, wrote this piece for The Conversation. Colorado State has recently joined The Conversation, an independent collaboration between editors and academics that provides informed news analysis and commentary to the general public, as a partner institution, and the list of participating faculty and researchers is expanding every day.
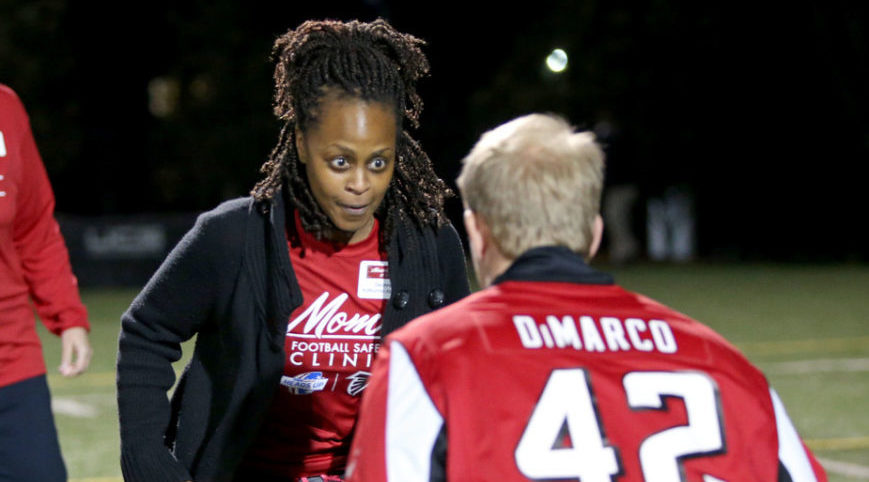
A mother from suburban Atlanta attending an educational session about concussions with Falcons fullback Patrick DiMarco in 2014. Jason Getz/AP
As Superbowl LI between the Atlanta Falcons and the New England Patriots approaches, football fans reflect on a season of intense competition, hard-fought battles and the tenacity of elite professional athletes. Among the over 100 million fans watching the game this Sunday will be approximately three million youth athletes who play the game themselves.
Entangled in the enthusiasm and attention to professional football is the conversation of concussive injury and how playing professional football is related to brain injuries, neurocognitive problems and neurodegenerative diseases such as Parkinson’s, Alzheimer’s and Chronic Traumatic Encephalopathy (CTE).
The National Football League has taken steps to protect their players from head injuries, such as changing rules and improving equipment, yet as the Wall Street Journal reports, rates in 2015 declined only slightly.
And while most of the media attention is directed at professional athletes, concussion and brain injuries are also a concern for soldiers in the military and for millions of youth athletes. Rates of concussion in these groups have led researchers and medical professionals to identify concussion as a public health crisis.
As a prevention scientist, I’ve worked extensively with schools and community groups to change personal, social and environmental factors that contribute to unhealthy behaviors such as adolescent substance use, risky sexual behavior or violence. Many of the methods used to address those public health issues can be applied to youth concussions as well.
A widespread problem
About 56 percent of youth ages 6-17 play an organized sport, and the Centers for Disease Control estimates that each year in the United States, between 1.6 and 3.8 million youth suffer a concussion.
Growing media attention and new educational opportunities, such as the CDC’s Heads Up program, seek to inform and encourage reporting of concussion and include specific programs to help coaches, parents, health care providers and athletes learn about the signs of concussion and the need to report them. Research indicates, however, that youth athletes may still underreport concussion.
A survey of Massachusetts youth indicated that almost half of athletes who experienced concussion symptoms continued to play that day, and only one-third stopped playing and were checked by a doctor that day.
Hiding symptoms of concussion and continuing to play in sports can result in subsequent injury, delayed recovery, delayed access to treatment and risk of catastrophic injury. An Institute of Medicine and National Research Council report on youth concussion concluded young athletes face a “culture of resistance” to reporting. It found research is needed to understand individual and social factors that create this culture and how it can be changed.
My colleague, Alissa Wicklund, who leads the Regional Concussion Center at the Orthopaedic and Spine Center of the Rockies, and I have a research project to address these issues. The project is part of the MindMatters Challenge, funded by the National Collegiate Athletic Association (NCAA) and the Department of Defense (DOD), and focuses on three questions:
- What factors influence whether youth report concussion symptoms?
- How to characterize and measure the culture of resistance?
- How to change the culture of resistance?
Although much of the research in this NCAA-DOD initiative focuses on collegiate athletics or the military, or both, our team of developmental clinical psychologists and athletic trainers will work with middle and high school youth. The students will be from nine schools in northern Colorado. The research team will try to shape the early knowledge, attitudes, beliefs and behaviors around concussion reporting.
We know characteristics of youth athletes, such as the knowledge they have about concussion, their attitudes about how serious symptoms are and their beliefs that if they report a concussion they will let the team down, all influence whether they will report concussion symptoms.
But to understand the culture of resistance, our study is gathering data about the knowledge, beliefs and attitudes of coaches, parents and peers – the key people in the athletes’ social networks that influence athletes’ decisions whether or not to report concussion symptoms.
We will study the environmental factors such as access to concussion materials and whether schools, districts or states have concussion reporting policies. While some studies have examined different factors independently, our study looks at them together to gain a fuller picture of the “culture” that middle school and high school athletes exist in.
Because we believe the culture may differ for girls and boys, in different schools or by sports and teams (girls’ volleyball vs. boys’ football), we will examine these subcultures and their influences on youth concussion reporting.
Involving stakeholders to change the culture
To change the culture, we are testing a process in which key members of the schools (students, teacher, coaches, trainers, parents) will learn about concussion, examining the data from their school. From there, the intent is to discuss what the data suggest is needed to change the culture, create an action plan for using evidence-based programs, practices or policies, and then implement those programs and policies in their schools. Rather than implementing identical programs at each school, the process emphasizes school-specific practices so schools will choose the interventions that are likely to work most efficiently and best for them.
Our intervention is based on empirically validated processes that have been used to change school and community “cultures” of substance use and violence.
Programs that teach about concussion are not likely to be sufficient, some studies have shown, and may in some cases have a negative effect on reporting behavior. We believe it will be important to take a broader approach that also addresses the emotional aspects of sport participation and nonreporting, the social pressures such as feeling embarrassed, letting the team down or being perceived as weak. We also need to look at the relationships athletes have with coaches and parents.

Karen Pulfer Focht/AP
Youth sports have many positive benefits that can last a lifetime. Keeping youths safe in sport should be a primary objective of all individuals involved in youth athletics. While changes in equipment, coaching, rules and style of play can all contribute to reducing the likelihood of sport-related concussions, trainers must also be aware of the social, emotional and behavioral factors that contribute to whether an athlete will disclose symptoms. The diagnosis and treatment of concussions is almost entirely dependent on athletes’ accurate reporting of symptoms to parents, trainers and coaches. Effectively addressing the public health concern of concussion non-reporting in youth sports will require the active involvement and dedicated efforts of parents, coaches, peers, teammates, administrators, athletic trainers and medical personnel.
This article was originally published on The Conversation. Read the original article.